Basel, Switzerland (UroToday.com) Dr. Piet Ost from Belgium discussed treatment of oligorecurrent prostate cancer after local therapy at the APCCC 2019 biennial meeting.
Dr. Ost notes that this is defined as a patient with a treated (and controlled) primary tumor, is naïve to systemic treatment, and has N1 or M1 metastasis. Currently, there is no consensus definition for oligometastatic disease. Typically, this is defined as five or less lesions, but different terminologies and lesion cut-offs are often used. The EORTC-ESTRO group is working on a consensus working definition that should be used in subsequent trials and studies. According to Dr. Ost, the future is a molecular definition, which is a GAP6 Movember initiative.
According to the most recent definition of the European Association of Urology Guidelines, restaging after radical prostatectomy should include a PSMA PET-CT if the PSA level is >0.2 ng/mL and if the results will influence subsequent treatment decisions (strength – weak). For PSA recurrence after radiation therapy, a PSMA PET-CT (or fluciclovine PET or choline PET) should be performed in patients fit for curative salvage treatment (strength – strong). Based on several studies, Dr. Ost notes that we essentially know where these recurrences will be: for both choline PET (median PSA 3 ng/mL) and PSMA PET (median PSA 2.6) more than 50% of recurrences will be in the pelvic lymph nodes.
Two years ago, Dr. Ost mentioned that there was poor evidence for metastasis-directed therapy for oligometastatic disease, with no prospective evidence. However, since then, phase II trials of metastasis directed therapy vs observation have been reported. Dr. Ost’s own trial randomized 62 patients with asymptomatic prostate cancer that had had a biochemical recurrence after primary treatment with curative intent, three or fewer extracranial metastatic lesions on choline PET-CT, and serum testosterone levels > 50 ng/mL to either surveillance or metastasis-directed therapy of all detected lesions (surgery or stereotactic body radiotherapy)1. At a median follow-up of 3 years, the median ADT-free survival was 13 months for the surveillance group and 21 months for the metastasis-directed therapy group (HR 0.60, 80% CI 0.40-0.90):
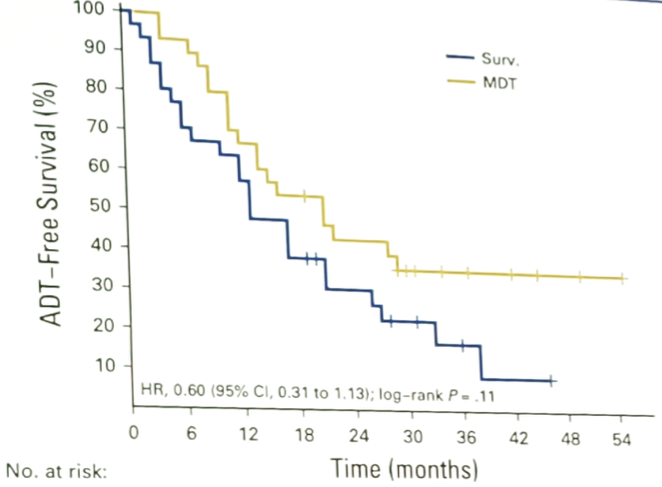
Importantly, there were no grade 2 to 5 toxicities in this trial. Furthermore, these results have also been corroborated in other tumor types, such as lung cancer where there has also been an OS benefit. Based on these findings, Dr. Ost suggested that metastasis-directed therapy should be explored further in phase III trials. In additional work from his group that was recently submitted for peer-review, Dr. Ost suggests that metastasis-directed therapy is also cost-effective: at a level of 1,000 euros per QALY, there is a 50% probability that metastasis-directed therapy is more cost-effective than either ADT or surveillance.
Dr. Ost concluded his presentation with several summary take-home points:
- Phase II trials indicate that metastasis-directed therapy is feasible, well-tolerated and improves biochemical response and progression free survival compared to observation
- Metastasis-directed therapy in other tumor types has demonstrated an improvement in OS
- Metastasis-directed therapy should not be considered standard of care based on phase II trials, but should be further evaluated in phase III trials, which are underway
Presented by: Piet Ost, MD, PhD, Ghent University Hospital, Ghent, Belgium
Written by: Zachary Klaassen, MD, MSc – Assistant Professor of Urology, Georgia Cancer Center, Augusta University/Medical College of Georgia, Tiwtter: @zklaassen_md at the 2019 Advanced Prostate Cancer Consensus Conference (APCCC) #APCCC19, Aug 29 – 31, 2019 in Basel, Switzerland
Reference:
1. Ost P, Reynders D, Decaestecker K, et al. Surveillance of Metastasis-Directed Therapy for Oligometastatic Prostate Cancer Recurrence: A Prospective, Randomized, Multicenter Phase II Trial. J Clin Oncol 2018 Feb 10;36(5):446-453.
