Basel, Switzerland (UroToday.com) In the past, androgen deprivation therapy (ADT) was the only available option for metastatic prostate cancer. When looking at data published 15 years ago, approximately 4.4-7% of metastatic patients lived for more than 10 years.1,2 The independent predictors of survival were lower PSA, low volume disease, lack of pain, and lower Gleason score.1 However, in the last 10 years, there has been tremendous progress in the available treatment options for metastatic prostate cancer patients (Figure 1). Serial systemic therapy with combinations of ADT with chemotherapy, abiraterone, or enzalutamide, and other therapies are now standard of care. Local and metastases directed therapy are still considered investigational at present, but earlier interventions in certain circumstances have shown to improve outcomes.
When assessing and comparing older and newer cohorts of metastatic prostate cancer patients’ outcomes have improved significantly in the last 10 years, with 5-year overall survival rates increasing from 10% between 2004 and 2007 to 26% between 2010-2013.3
Figure 1- Significant progress in the treatment option for metastatic prostate cancer in the last 10 year:
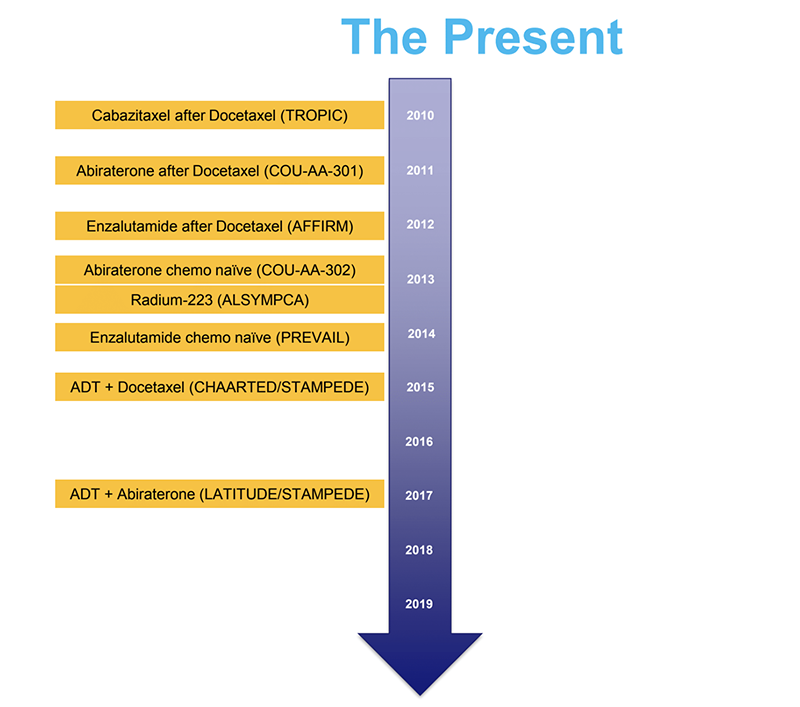
It is difficult to predict what the future holds in this field, but we can certainly imagine. Dr. Oh predicts that immunotherapy will gain a substantial role in the treatment of these patients and that we might even be able to think of the word “cure,” although we are still a long way away. For example, the number of search results for the combination of “cancer” and “cure” in PubMed has risen substantially in the past years (Figure 2).
Figure 2 – PubMed citations of the words “cancer” and “cure”:
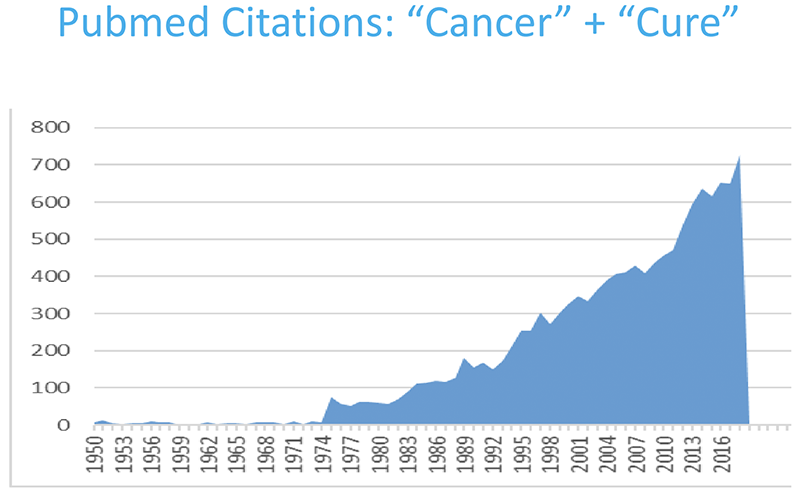
The standard approach currently used for the treatment of metastatic prostate cancer incorporates monotherapy of one single advanced drug until resistance develops, and then treatment is switched. Some of the analyzed combinations have shown excess toxicity. However, by designing a rapidly-cycling, non-cross-reactive treatment regimen we might be able to:
- Treat intrinsic heterogeneity
- Prevent drug resistance
- Increase long term disease control
- Minimize toxicity
This management strategy is called Prostate Cancer Intensive, Non-Cross-Reactive Therapy (PRINT) for metastatic castrate-resistant prostate cancer (mCRPC). Dr. Oh described an ongoing study at Mount Sinai using this principle in mCRPC patients (Figure 3).
Dr. Oh concluded his talk summarizing some of his personal predictions for the future of metastatic prostate cancer. First, the molecular characterization of tumors will be increasingly relevant as newer targeted drugs are developed. Second, Immunotherapy in metastatic prostate cancer will be more effective. Third, more combination therapies (local and systemic) will be used. Lastly, Functional “cures” of metastatic prostate cancer will become more common. Dr. Oh believes that a cure is possible in metastatic prostate cancer if our definition is flexible.
Figure 3: PRINT ongoing study for mCRPC patients:
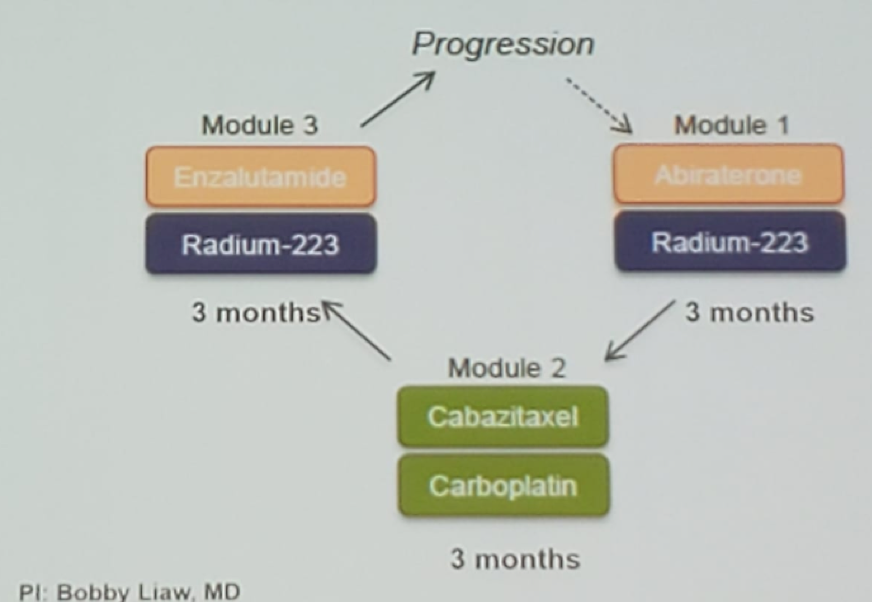
Presented by: William Oh, MD, Professor, Medicine, Hematology, Urology and Medical Oncology, Mount Sinai Hospital, New York, USA
Written by: Hanan Goldberg, MD, Urology Department, SUNY Upstate Medical University, Syracuse, New-York, USA @GoldbergHanan at the 2019 Advanced Prostate Cancer Consensus Conference (APCCC) #APCCC19, Aug 29 – 31, 2019 in Basel, Switzerland
References:
- Tangen CM, Faulkner JR, Crawford ED, et al. Ten-Year Survival in Patients with Metastatic Prostate Cancer. Clinical Prostate Cancer. 2003;2(1):41-45.
- Klaff R, Berglund A, Varenhorst E, Hedlund PO, Jonler M, Sandblom G. Clinical characteristics and quality-of-life in patients surviving a decade of prostate cancer with bone metastases. BJU international. Jun 2016;117(6):904-913.
- Francini E, Gray KP, Shaw G, et al. Impact of new systemic therapies on overall survival (OS) of patients (pts) with metastatic castration resistant prostate cancer (mCRPC) in a hospital-based registry. Journal of Clinical Oncology. 2018;36(6_suppl):203-203.
