Barcelona, Spain (UroToday.com) Inhibition of angiogenesis using either tyrosine kinase inhibitors against the VEGF receptor (e.g. pazopanib, axitinib, cabozantinib) or antibodies against circulating VEGF (e.g. bevacizumab) have been effective therapies in advanced renal cell carcinoma. Preclinical data has previously implicated endoglin, a receptor on the surface of endothelial cells, as a resistance mechanism for VEGF/VEGFR targeted therapy. Targeting endoglin with the monoclonal antibody TRC105 has been shown to potentiate VEGF/VEGFR inhibition in preclinical models. A phase 1b dose-escalation trial1 of TRC105 recently showed a 29% partial-response rate in heavily pre-treated metastatic renal cell carcinoma (mRCC) patients.
In this poster, Dr. Toni Choueiri and colleagues present data from the phase II TRAXAR study (NCT01806064) that randomized mRCC patients who had progressed after at least 1 VEGF inhibitor in a 1:1 fashion to receive either axitinib 5 mg BID or axitinib plus TRC105 10 mg/kg weekly. The primary endpoint of this study was progression-free survival by RECIST criteria, and secondary endpoints were overall response rate and safety.
Patients were well-balanced between the cohorts. Approximately 90% of patients had undergone prior nephrectomy, ~10% had received prior immunotherapy, and ~60% had received just one prior cancer therapy.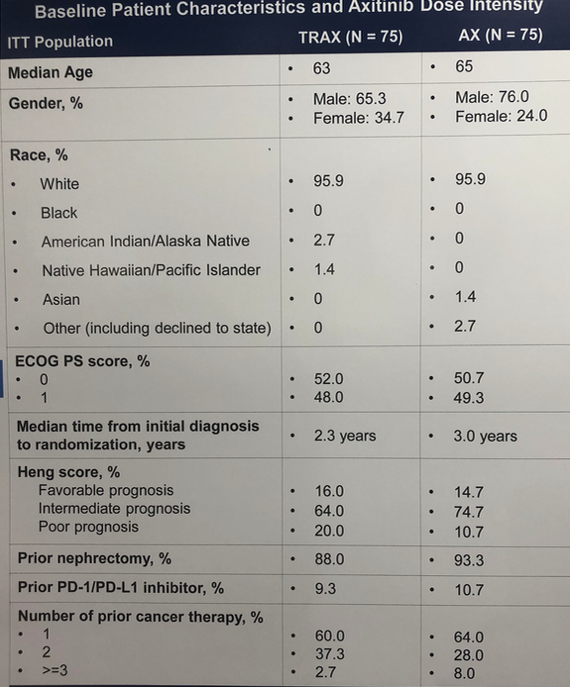
Regarding the primary endpoint, treatment with axitinib plus TRC105 did not provide any benefit for progression-free survival relative to axitinib monotherapy (HR 1.42, 95% CI: 0.88-2.30, P = 0.15). There was no benefit for combination therapy with regards to overall response rate.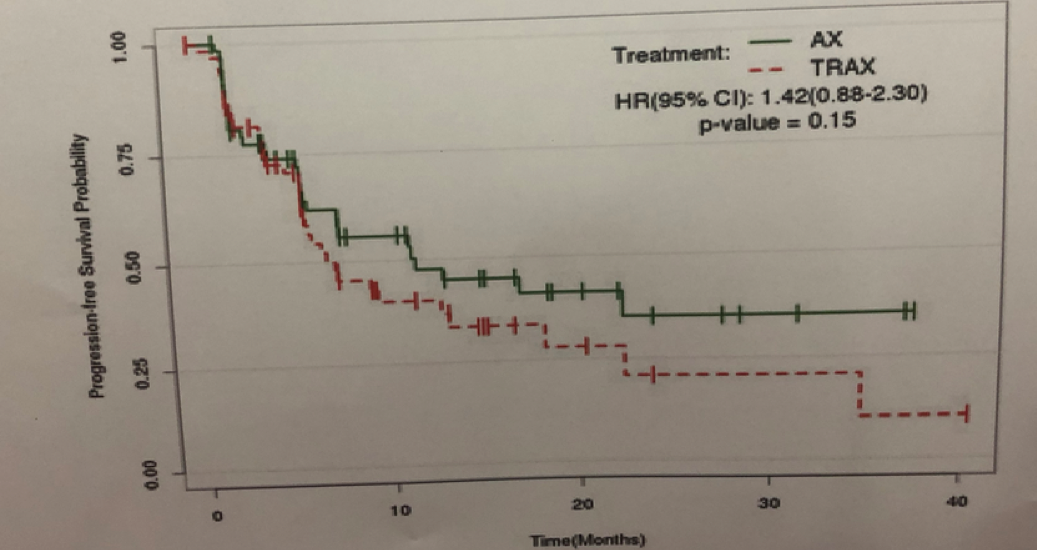
Subgroup analysis by clinical parameters did not reveal any particular patient group that uniquely benefitted from the addition of endoglin inhibition.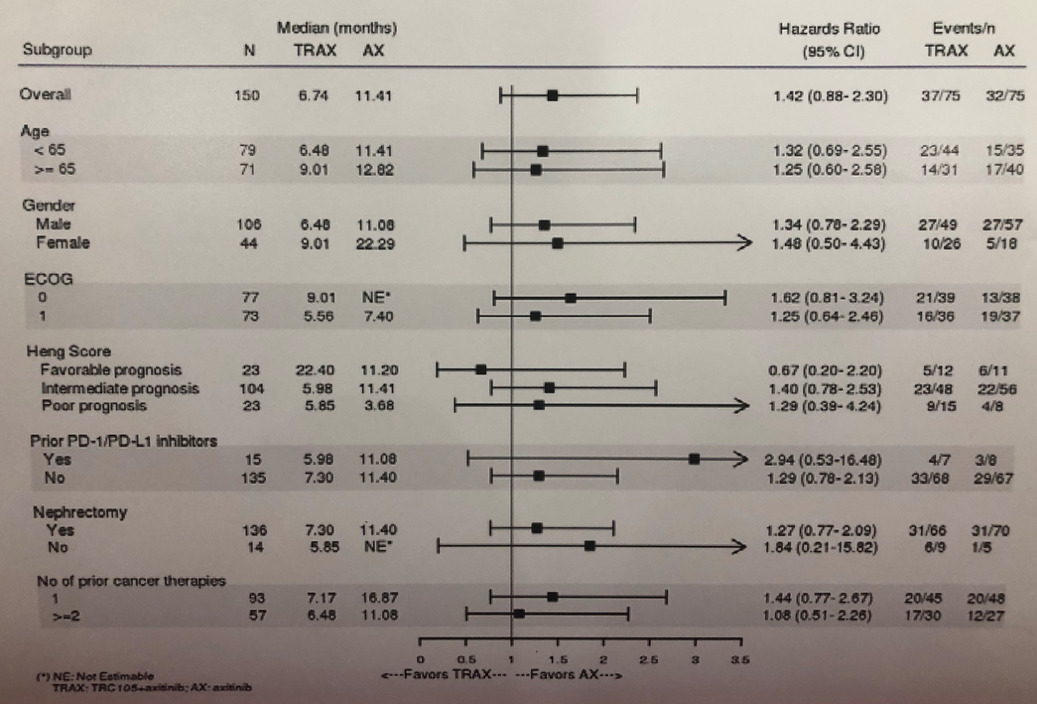
Combination therapy was tolerated relative to axitinib, with 20% of patients in the combination arm discontinuing therapy due to treatment-related adverse effects, and 13% of axitinib patients discontinuing therapy for the same reason. Side effects were more frequent with TRC105 + axitinib therapy, most notably with regards to grade 3 anemia and diarrhea. Therapy was on target, as all patients receiving TRC105 developed symptoms of Osler-Weber-Rendu syndrome.
In summary, the combination of the endoglin-targeting agent TRC105 in combination with axitinib did not improve mRCC progression-free survival in this randomized phase 2 study. In the setting of prior data showing no improvement in patient outcomes with TRC105 plus bevacizumab and a hazard ratio in this study favoring axitinib monotherapy, further work is required to understand if endoglin remains a targetable resistance mechanism to VEGF/VEGFR therapy in mRCC.
Presented by: Toni Choueiri, MD, Professor of Medicine and Director of Genitourinary Oncology at the Dana-Farber Cancer Institute and Harvard Medical School, Boston, Massachusetts, USA
Written by: Alok Tewari, MD, PhD, Medical Oncology Fellow at the Dana-Farber Cancer Institute, at the 2019 European Society for Medical Oncology annual meeting, ESMO 2019 #ESMO19, 27 Sept – 1 Oct 2019 in Barcelona, Spain
